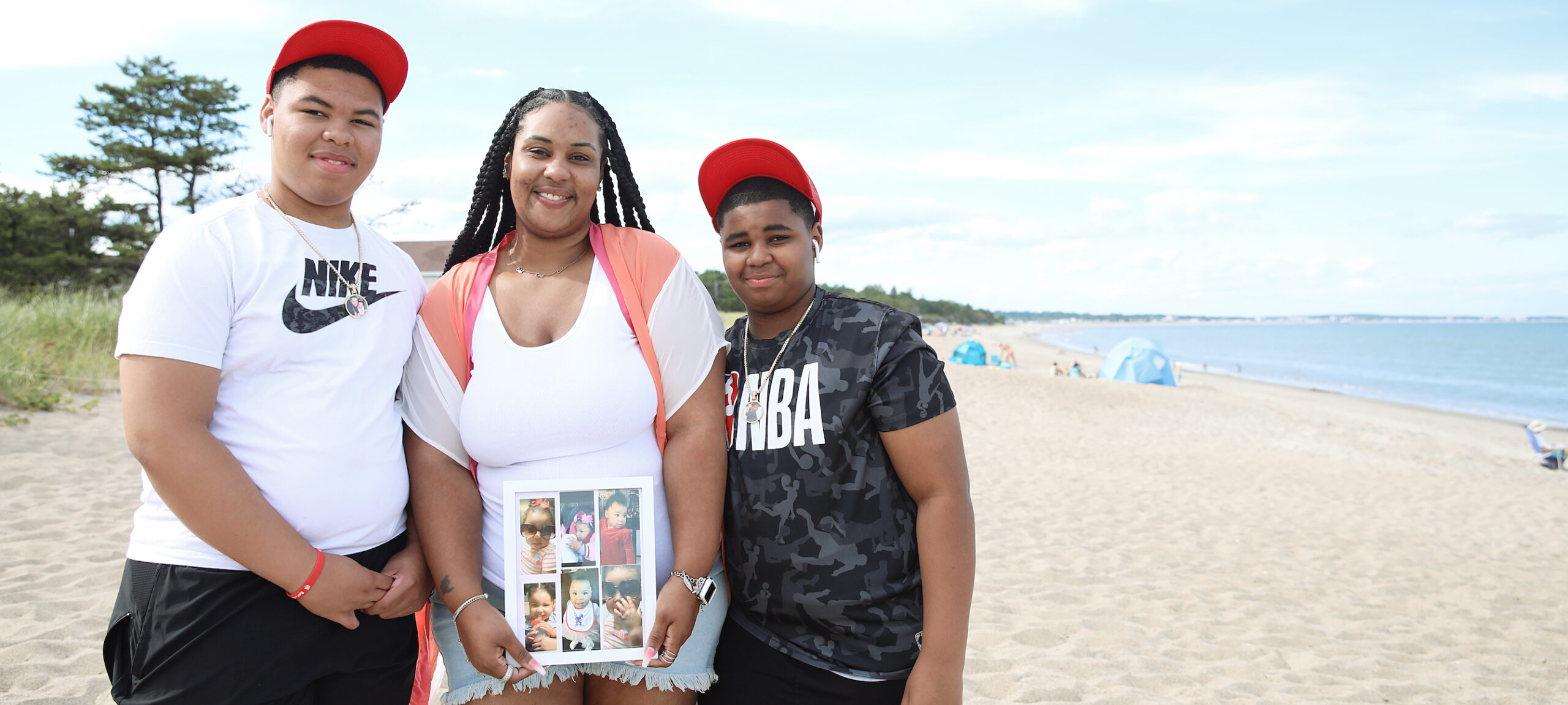
The Thompson Family
Cori was a blessing to all that knew her. She had big beautiful curly hair, which she loved to adorn with huge bows. She was well mature for her age and knew just how to make her big brothers smile.

The Austin Family
The three of us were holding him and it was an extremely peaceful transition. I felt very similar emotions as I did when he was born, which was just essentially an immense amount of love, only paired with sorrow instead of joy.

The Schultz Family
For our family it was like a bomb went off. Our amazing life was blown apart. We were shellshocked, and also desperate to believe that we could find some experimental treatment that would save her or give her more time.

The Bares Family
Laurel died in our bed between my husband and I in the early morning of June 15, 2018. We were up with her the night before, singing songs and reading and telling her she was the love of our life.

The Ojeda Family
Jayden loved love, he loved life, and most importantly he loved his family and made sure everyone knew that. He was the most caring, selfless, sweet teenager that you can possibly meet

The Fromwiller Family
Chace’s mom told us that the news of his DIPG diagnosis completely rocked their world; it felt like their life completely stopped when everyone else’s kept going. They have experienced anger, sadness, and numbness at times.

The Jarboe Family
June was an amazingly spirited girl. She was the happiest, always, despite life's circumstances. She completed treatment with beauty and grace. She is and was our angel and she will forever be the strongest person we have ever met.

Alister’s Family
Alister was born with a rare & complex genetic disorder called Alagille Syndrome, which affected his liver and heart. Out of nowhere, on July 8, 2019, Alister was diagnosed with acute lymphoblastic leukemia.

The Rouleau Family
So many people say that Eliana was a bright light in this world. There was a sense of peace and joy when being with her. She loved life, and did not let her cancer stop her from exploring the world and enjoying all things.

The Sweger-Nesbits
William was always putting people before himself and he lived each day with a positive attitude and a smile on his face. Even on his really difficult days. Walking out of that hospital without my son was the most difficult thing I have ever had to do, and I continue to put one foot in front of the other every day since. I honor him by doing my best to live the same.


